Early Diabetes Warning Signs: Understanding Dark Skin Patches and Blood Sugar Symptoms
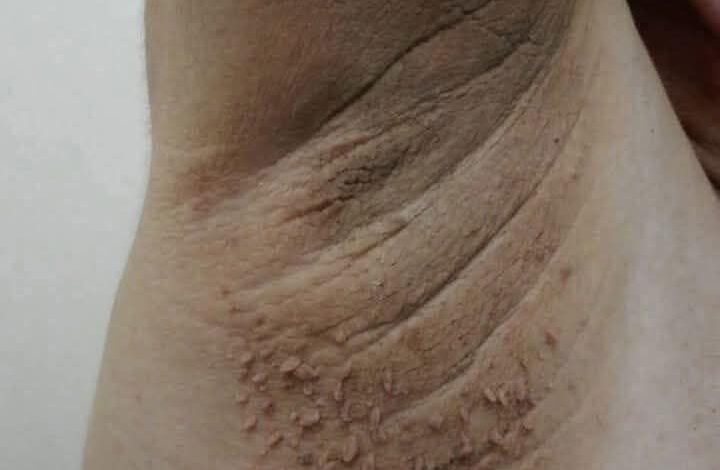
Diabetes prevention begins with recognizing early warning signs that many people overlook. One of the most visible yet misunderstood symptoms involves dark, velvety skin patches that appear on the neck, underarms, or other body areas. These patches, often mistaken for poor hygiene, may actually signal important changes in blood sugar levels and insulin resistance.
Understanding these early diabetes symptoms can be crucial for preventing type 2 diabetes and implementing effective diabetes management strategies before serious complications develop.
Understanding Acanthosis Nigricans: A Key Diabetes Warning Sign
Acanthosis Nigricans represents a significant skin condition that serves as an early indicator of metabolic changes in the body. This condition manifests as darkened, thickened patches of skin with a distinctive velvety texture, most commonly appearing in areas where skin folds occur.
Common Locations for Acanthosis Nigricans:
Primary Areas:
- Neck region (most frequent location)
- Underarm areas
- Groin and inner thigh regions
- Behind the knees
- Elbow creases
Secondary Locations:
- Knuckles and finger joints
- Lip areas
- Eyelid regions
These patches cannot be removed through washing or scrubbing, distinguishing them from actual dirt or poor hygiene. The affected areas may feel soft to the touch and occasionally exhibit increased hair growth patterns.
Medical Causes and Risk Factors for Acanthosis Nigricans
Healthcare professionals recognize Acanthosis Nigricans as a visible manifestation of underlying metabolic disorders rather than a standalone skin disease. Understanding these root causes helps in early diabetes detection and prevention.
Primary Medical Causes:
Insulin Resistance and Prediabetes:
Insulin resistance occurs when body cells become less responsive to insulin, leading to elevated blood glucose levels. This condition often precedes type 2 diabetes development and frequently presents with Acanthosis Nigricans as an early warning sign.
Obesity and Weight Management Issues:
Excess body weight, particularly in children and adolescents, significantly increases the risk of developing both insulin resistance and associated skin changes. Childhood obesity has become a growing concern for diabetes prevention specialists.
Hormonal Disorders:
Various endocrine conditions can trigger Acanthosis Nigricans, including:
- Polycystic ovary syndrome (PCOS)
- Thyroid disorders
- Adrenal gland abnormalities
- Growth hormone disorders
Genetic Predisposition:
Family history of diabetes, metabolic syndrome, or insulin resistance increases individual risk factors for developing these skin changes.
Expert Medical Opinion on Diabetes Prevention
Medical professionals emphasize the importance of recognizing these early diabetes symptoms for effective prevention and treatment. Endocrinologists and dermatologists frequently collaborate to identify patients at risk for metabolic disorders.
Recent medical research indicates that children and adults presenting with Acanthosis Nigricans should undergo comprehensive diabetes screening, including:
- Fasting blood glucose tests
- Hemoglobin A1C measurements
- Glucose tolerance testing
- Insulin level assessments
Healthcare providers stress that these skin changes are typically painless and non-itchy. If affected areas become irritated, red, or painful, alternative skin conditions such as eczema or contact dermatitis should be considered.
Blood Sugar Testing and Diabetes Screening Methods
Regular blood sugar monitoring plays a crucial role in diabetes prevention and early detection. Several testing options are available for individuals concerned about potential diabetes symptoms.
Professional Testing Options:
Medical Laboratory Testing:
- Comprehensive metabolic panels
- Fasting glucose measurements
- Oral glucose tolerance tests
- Hemoglobin A1C assessments
Pharmacy-Based Testing:
Many pharmacies offer convenient blood glucose screening services, providing immediate results and diabetes risk assessment.
Home Testing Equipment:
Blood glucose meters allow for regular monitoring and can help track blood sugar patterns over time. These devices are particularly valuable for individuals with prediabetes or family history of diabetes.
Recommended Testing Schedule:
- Annual screening for adults over 45
- More frequent testing for high-risk individuals
- Immediate testing when symptoms appear
- Regular monitoring for those with prediabetes
Differential Diagnosis: Other Skin Conditions
Medical professionals must distinguish Acanthosis Nigricans from other skin conditions that may present similar appearances. Accurate diagnosis ensures appropriate treatment and addresses underlying health concerns.
Terra Firma-Forme Dermatosis (TFFD):
This benign skin condition can mimic Acanthosis Nigricans but differs in several key ways:
- Can be removed with alcohol-based solutions
- Not associated with metabolic disorders
- Typically affects different body areas
- Responds to topical treatments
Diagnostic Testing:
Healthcare providers may use the “alcohol swab test” to differentiate between these conditions. If dark patches can be removed with 70% isopropyl alcohol, TFFD is likely the diagnosis rather than Acanthosis Nigricans.
When to Seek Medical Attention for Diabetes Symptoms
Recognizing when to consult healthcare professionals can significantly impact diabetes prevention and treatment outcomes. Early medical intervention often prevents progression to type 2 diabetes.
Immediate Medical Consultation Recommended:
Sudden Onset Symptoms:
- Rapid development of dark skin patches
- Spreading or enlarging affected areas
- Changes in patch texture or appearance
Associated Diabetes Symptoms:
- Increased thirst and frequent urination
- Unexplained weight loss or gain
- Persistent fatigue or weakness
- Slow-healing wounds or infections
- Blurred vision or visual changes
Risk Factor Considerations:
- Family history of diabetes or metabolic syndrome
- Personal history of gestational diabetes
- Polycystic ovary syndrome (PCOS)
- High blood pressure or cholesterol levels
Diabetes Prevention Through Lifestyle Modifications
Effective diabetes prevention often involves comprehensive lifestyle changes that address underlying insulin resistance and metabolic risk factors. These modifications can also help reduce the appearance of Acanthosis Nigricans.
Nutritional Strategies:
Diabetes-Friendly Diet Plans:
- Low-glycemic index foods
- Increased fiber intake through vegetables and whole grains
- Lean protein sources
- Healthy fats from nuts, seeds, and fish
- Portion control and meal timing
Foods to Limit:
- Sugary beverages and processed foods
- Refined carbohydrates
- High-sodium processed meals
- Trans fats and excessive saturated fats
Physical Activity Recommendations:
Cardiovascular Exercise:
- Minimum 150 minutes of moderate activity weekly
- Walking, swimming, or cycling
- Interval training for improved insulin sensitivity
Strength Training:
- Resistance exercises 2-3 times weekly
- Muscle building for improved glucose metabolism
- Bodyweight exercises for accessibility
Weight Management Strategies:
Sustainable weight loss through caloric balance and increased physical activity can significantly improve insulin sensitivity and reduce diabetes risk.
Medical Treatment Options for Acanthosis Nigricans
While addressing underlying causes remains the primary treatment approach, medical professionals may recommend additional interventions for managing the appearance of Acanthosis Nigricans.
Topical Treatments:
Prescription Medications:
- Retinoids for skin cell turnover
- Topical corticosteroids for inflammation
- Vitamin D analogs
- Alpha hydroxy acids
Over-the-Counter Options:
- Exfoliating treatments
- Moisturizers with urea or lactic acid
- Gentle cleansing products
Systemic Treatments:
For cases related to insulin resistance, healthcare providers may prescribe:
- Metformin for blood sugar control
- Other diabetes medications as appropriate
- Hormonal treatments for underlying conditions
Long-Term Health Monitoring and Diabetes Management
Individuals diagnosed with Acanthosis Nigricans require ongoing medical supervision to monitor for diabetes development and other metabolic complications.
Regular Health Screenings:
Blood Work Monitoring:
- Quarterly or semi-annual glucose testing
- Annual comprehensive metabolic panels
- Lipid profile assessments
- Kidney function evaluations
Physical Examinations:
- Regular skin assessments
- Blood pressure monitoring
- Weight and BMI tracking
- Eye examinations for diabetes complications
Preventive Care Strategies:
Maintaining regular healthcare visits allows for early detection of diabetes progression and implementation of appropriate interventions.
Conclusion: Proactive Diabetes Prevention and Health Awareness
Dark skin patches, particularly Acanthosis Nigricans, serve as important early warning signs for diabetes and metabolic disorders. While these symptoms may seem cosmetic, they often indicate significant underlying health changes that require medical attention.
Early recognition and appropriate medical evaluation can lead to effective diabetes prevention strategies and improved long-term health outcomes. Combining regular health screenings with lifestyle modifications provides the best approach for managing diabetes risk factors.
Individuals experiencing these symptoms should consult healthcare professionals for proper diagnosis and treatment planning. With appropriate medical care and lifestyle changes, many people can successfully prevent type 2 diabetes and maintain optimal health.
This information is for educational purposes only and should not replace professional medical advice. Always consult with healthcare providers for proper diagnosis and treatment of medical conditions.